
Managing Stress from a Holistic Health Coach’s Point of View
By: Lisa Altieri, RN, CHHC
A stroke can have very serious physical, as well as psychological, consequences for the survivor. The resulting physical difficulties can place considerable demands on both the survivor as well as the caregiver(s). The lifestyle one is accustomed to living can change suddenly, leaving the stroke survivor and their caregiver (s) significant challenges to overcome. Family roles can suddenly change overnight.
Survivors may require assistance with many daily activities, personal hygiene, bathing, dressing, feeding etc. One goes from living independently to possibly depending on someone for many of their basic needs. This can change a person’s image of themselves and their outlook on life. They may feel that they are a burden to their caregivers. Family members who have their own lives and responsibilities, may now be responsible for the care of the stroke survivor. Both survivors and caregivers will likely be faced with emotional challenges that should be addressed.
Following a stroke, it is essential to be aware of potential risk factors for your health and also the potential for another stroke. This blog series will take you through an educational landscape on such factors like, stress, physical inactivity, high blood pressure, unhealthy diet, and high cholesterol.
Stress. The word that so many of us experience on a daily basis. Yet, how can one productively channel that stress, especially after experiencing a stroke?
Traditionally, an increased risk of stroke has primarily been linked to high blood pressure and/or cholesterol, unhealthy diet, and physical inactivity. However, researchers have highlighted the importance of understanding “modifiable risk factors, including stress and negative emotions, is needed given the aging population and increasing burden of stroke.”
“Stress and negative emotions activate the hypothalamic-pituitary-adrenal axis… and this activation of the brain’s stress center influences blood clotting, among a number of other effects.” Furthermore, a study reported in the American Heart Association’s journal Stroke revealed depressive symptoms and also chronic stress can increase the risk of having a stroke or a transient ischemic attack (TIA). In this study, over 6,500 adults between the ages of 45-84 (53% women), completed a questionnaire about chronic stress, hostility and depression for the course of two years. None of the participants had cardiovascular disease when the study was initiated. Over 8.5 years later, there were 147 strokes and 48 TIA’s. Here are the numbers and how psychological stressors impacted their risk of stroke:
- 86% more likely to have a stroke or TIA if they had depression
- 59% more likely to have a stroke or TIA if they had chronic stress
- More than twice as likely to have a stroke or TIA if they had hostility
Long term stress, or chronic stress is indeed a risk factor for a stroke. A research study found that people who had experienced stress previously (over a year), were nearly four times more likely to have stroke, compared to others who were not under similar stress. This stress may have included financial, relationship, or work… to name a few.
So, … now that we know how much of an impact stress can have on our health, let’s take a look at some important techniques and advice for the survivor, as well as the caregiver that may help heal the mind and body after a stroke.
Holistic Interventions to Combat Stress

Balance. Stay grounded and remain focused on your goals. This may mean setting boundaries with your friends and family. So if this is something that you are experiencing difficulty doing, check out this article. If you do not have your goals or intentions in writing, and the thought of this is overwhelming to you, perhaps start with a vision board class. Maybe you feel like you may need more of a one on one approach. You may find that seeking out a reputable Health Coach is just what you need. No matter how you chose to go about it, staying balanced will give you the energy you need to complete your tasks, while caring for yourself.
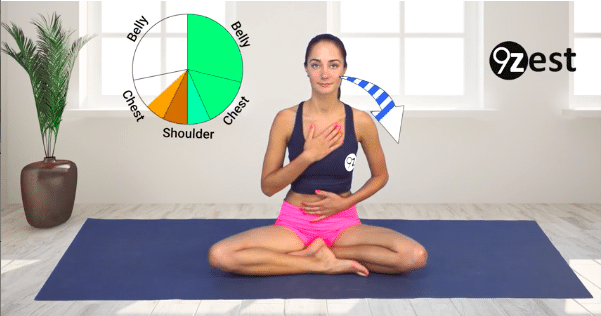
Breathing. Stress is inevitable, and a part of all of our lives. How we chose to handle it, is a predictor of our overall health. Our Autonomic Nervous System is part of the peripheral nervous system. It controls and regulates the internal organs without conscious effort. Two of the 3 subdivisions are the; the Sympathetic Nervous System (SNS), the Parasympathetic Nervous System (PNS). When we are stressed the Sympathetic Nervous System responds and is referred to as the “fight or flight response.” This surge of hormones results in many physiological changes including; tense muscles, sweating, increased heart rate, pale or flushed skin, trembling, and many other changes. After a while, this has an effect on the body that contributes to the health problems associated with chronic stress. Our Parasympathetic Nervous System is referred to as our “rest and digest” system. When the PNS is aroused, it produces a feeling of relaxation and calm in the body and mind. The PNS decreases heart rate, lowers blood pressure as well as other physiological changes. We can restore the balance by lighting up our PNS. One way to do this is with simple breathing exercises, here are a few good ones to help you get started.

Encouraging Independence. It may very difficult and at times, scary, to encourage independence. Safety, of course, should always come first. However, the survivor is usually capable of doing more than the caregiver may assume. Promoting their independence, while being safe, can be very helpful through the coping process. Speak to your physical therapist about safety tips to help you empower your survivor.
Joining a Support Group. Support groups can provide a tremendous amount of support and emotional aid to both the survivor and caregiver(s). Think of a support group like a community that you can turn to at any time. This support will allow you to speak to other individuals who are dealing with similar challenges and lifestyle changes. It’s a great way to communicate and engage with the community as it also serves as an educational platform. Consistent communication in a group setting can help you identify different treatments, devices, events, physicians, and more.


Sleep. A study found that decreased sleep (less than 7-8 hours) leads to elevated cortisol levels. Cortisol is a hormone that your adrenal glands produce in response to stress.
Meditation & Exercise. Just giving yourself 10 minutes a day to meditate, can help you control stress, decrease anxiety and improve overall relaxation. Additionally, physical activity has been shown to lower stress. There is a scientific reason why we “feel good” after we exercise. Exercise increases your brains endorphins (the feel-good hormones)! Regular exercise can help increase self-confidence and lower symptoms associated with mild depression and anxiety.

Reducing stress is VITAL to our health and well-being. Let’s take that step together towards a healthier and happier life!
